Press Releases
A decades-long decline in the breast cancer death rate continues, but has begun to slow in recent years, while breast cancer incidence rates continue to inch up. These trends are outlined in Breast Cancer Statistics, 2019-2020, the latest edition of the American Cancer Society’s biennial update of breast cancer statistics in the United States, published in CA: A Cancer Journal for Clinicians, and the accompanying Breast Cancer Facts & Figures.
Breast cancer is the most common cancer (excluding skin cancers) diagnosed among U.S. women and is the second leading cause of cancer death among women after lung cancer. In 2019, approximately 268,600 new cases of invasive breast cancer will be diagnosed among U.S. women, and 41,760 women will die from the disease.
The overall breast cancer death rate has decreased consistently since 1989, attributed both to improvements in early detection (through screening as well as increased awareness of symptoms) and treatment for a total decline of 40% through 2017. As a result of this decline, 375,900 breast cancer deaths have been averted in U.S. women through 2017.
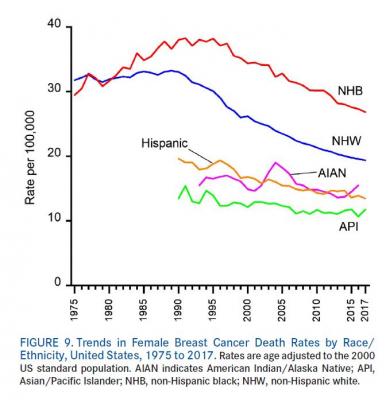
The latest data shows that the pace of the mortality decline has slowed in recent years—from a drop of 1.9% per year during 1998 through 2011 to 1.3% per year during 2011 through 2017, largely driven by the trend in white women. Consequently, the black-white disparity in breast cancer mortality that widened over the past three decades has remained stable since 2011. Nevertheless, in the most recent period (2013-2017), the breast cancer death rate was 40% higher in black women versus white women, despite slightly lower incidence rates. This disparity is magnified among black women under 50, among whom the death is rate double that of whites.
In the most recent 5-year period (2013-2017), the breast cancer death rate declined by 2.1% per year in Hispanics/Latinas, 1.5% per year in blacks, 1.0% per year in whites, and 0.8% per year in Asians/Pacific Islanders, and was stable in American Indians/Alaska Natives. However, mortality rates are no longer declining for black women in Colorado and Wisconsin and for white women in Nebraska, Texas, and Virginia.
Meanwhile, the breast cancer incidence rate has continued to slowly increase by 0.3% per year since 2004, largely because of rising rates of local stage and hormone receptor-positive (HR+) disease. The increase in rates of HR+ breast cancer is likely driven in part by increasing prevalence of excess body weight and declining fertility rates – risk factors that are more strongly associated with this subtype. In contrast, incidence rates have decreased for hormone receptor-negative breast cancer, which is associated with poorer survival.
During 2016-2017, breast cancer was the leading cause of cancer deaths (surpassing lung cancer) among black women in six states (Arizona, Colorado, Florida, Georgia, Mississippi, and South Carolina), as well as among white women in Utah. In four other states (Alabama, Massachusetts, New York, and Texas), the numbers of breast and lung cancer deaths among black women were similar.
“We can’t say for sure what the reasons are for the slowing of the decline in breast cancer mortality. It could be due in part to the slight increase in incidence since 2004, as well as a sign that optimal breast cancer treatment has become more widespread, particularly among white women,” said Carol DeSantis, MPH, lead author of the report. “However, more can and should be done to ensure that all women have access to quality care to help eliminate disparities and further reduce breast cancer mortality.”
Other findings from the report:
- During 2012 through 2016, breast cancer incidence rates increased among Asians/Pacific Islanders (1.5% per year), American Indians/Alaska Natives (0.8% per year), and blacks and whites (both 0.5% per year), but were relatively stable among Hispanic/Latina women.
- The lifetime risk of a breast cancer diagnosis is now rounded to 13% (12.8%; previously 12.4%), which still equates to about 1 in 8 women diagnosed with breast cancer in her lifetime.
- The ten-year probability of a breast cancer diagnosis is highest for women in their 70s (4%), whereas the 10-year risk of breast cancer death is highest in women in their 80s (1%).
- Among women 50 and older, rates of ductal carcinoma in situ (DCIS) increased more than 11-fold between 1980 and 2008 (from 7 cases per 100,000 to 83), but decreased by 2.1% per year in the most recent time period (2012-2016), largely reflecting trends in the use of mammography, which increased from 29% in 1987 to 70% in 2000 and has since declined slightly.
- As of January 1, 2019, there were more than 3.8 million women with a history of breast cancer living in the United States. This estimate includes more than 150,000 women living with metastatic disease, three-quarters of whom were originally diagnosed with stage I, II, or III breast cancer.
- Higher breast cancer death rates in black women reflect a combination of factors that are difficult to parse, including later stage at diagnosis, unfavorable tumor characteristics, higher prevalence of obesity and pre-existing medical conditions, and less access to timely and high-quality prevention, early detection, and treatment services.
Article: Breast Cancer Statistics, 2019, DeSantis et al., CA: Cancer J Clin 2019; doi: 10.3322/caac.21583.